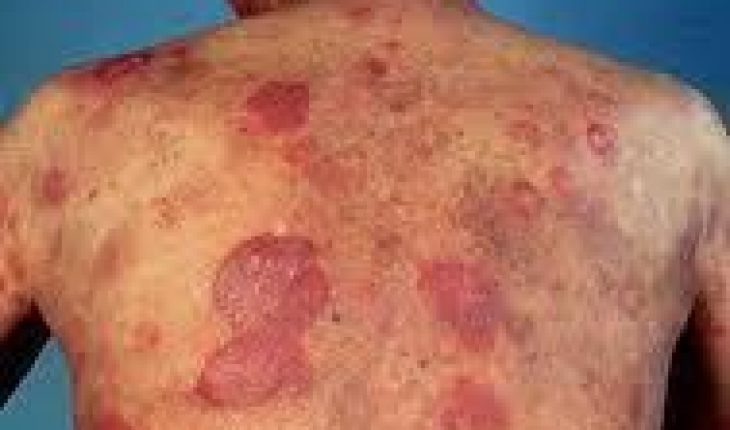
Mycosis fungoides, or as its known medically Cutaneous T cell lymphoma (CTCL), is not a single disease, but a group of cancers that attack the lymphatic system. It gets its name from its visual appearance, that of a mushroom-like fungus on the skin in its advanced stages. Mycosis fungoides evolve over time from malignant white blood cells called T-lymphocytes (T-cells). Their normal function is to fight infection, but when they themselves become infected they are sometimes drawn to the skin and deposited there, over time slowly becoming cancerous.
Causes of Mycosis fungoides
CTCL is sometimes misdiagnosed as the skin discolorations are similar to other less threatening diseases like eczema and psoriasis. There is no definite cause of Mycosis fungoides, but there are theories indicating it may be genetic. What is known is that it’s tied to several other diseases such as erythoderma and leukemia. It also targets males in the 40 to 50 year old bracket. Like every cancer it has stages indicating how serious it is. It begins on the surface and can invade whole organs including taking over the skin.
Symptoms
It is not uncommon for Mycosis fungoides to be misdiagnosed, especially when a patient is outside of the age group. Biopsies are the most conclusive test, but there are tell-tale signs to look out for.
- Patches on the skin – True to its name CTCL causes discolored patches, as it damages the skin. The patches tend not to be random in location, or size, but are clearly unusual in appearance.
- Itching – With the alteration of the skin comes the discomfort of itching. Most patients will have it mildly, but around 20% are often hit with severe periods of itching.
- Lesions – At this point the Mycosis fungoides is entrenched. The lesions can grow exponentially, and become sores and ulcers.
- Tumors – The ultimate sign that something is wrong, yet this milestone requires a biopsy to confirm the disease.
Cures
There is no fixed treatment for CTCL, nor is there an outright cure. Due to its slow growth, chemotherapy has little effect and surgery is generally off the table. Ultimately, the spread of the disease and the age of the patient, are the factors that determine the type of treatments.
- Steroids – Given in topical form, its application to the infected area helps reduce inflammation, promote increased oxygen flow, and blood vessel expansion. The downside is possible steroid side effects.
- Light – Regular sunlight is used to promote skin health due to its vitamin-D and calcium properties. Controlled it can cause remission. Another form of light treatment is Ultraviolet (UV) rays. Unlike regular sunlight that contains UV, this light it is used to kill the affected skin so that new patches can be reformed.
- Radiotherapy – Similar to UV treatments, radioactive elements are localized to the infected area, and kill the cells themselves instead of just the skin. At best the patient may experience removal, or a halt in spreading, but at worse this cure can create new complications.